The insurance claim process is complex and usually requires integrating with several legacy or external systems, and exchanging information between these systems and can be a long-running process over several months. Insurance organizations are often looking for ways to reduce processing time, improve service level agreements (SLAs) and streamline processes.
With Camunda powering your process orchestration, insurance organizations can create processes that can scale to any level, offering a distributed architecture designed for high transaction throughput. Camunda supports long running, end-to-end workflows using open-standard BPMN diagrams, allowing business units and IT teams to work together to improve automation in claims processing.
Orchestrating automobile claims with Camunda
Let’s assume that an insurance company has been tasked with streamlining the back office process for claims cases. The company focuses on the improvement of their Auto Claim Process. The first task is to research and document the current process. This includes determining which tasks are manual, what other departments and individuals are involved, and what additional systems are accessed in order to properly process claims. It is also important to gather the time required to complete various tasks as well as the costs involved: computer processing costs, working hour costs, and other associated costs.
In most cases, the following systems and departments are involved in the claims process:
- Claims Department and associated systems
- Policy Administration and associated systems
- Accounting – for payment processing – and associated systems
- Adjusters for determining automobile repair estimates
- Medical Adjusters for adjudicating associated medical claims
Note: This Glossary of Insurance Terms might help as you continue to read this post.
Once you have a solid understanding of the existing process, it is important to map out the claim process with the involved business units. Most organizations start simple and then continue to enhance the process to incorporate additional enhancements to your orchestration.
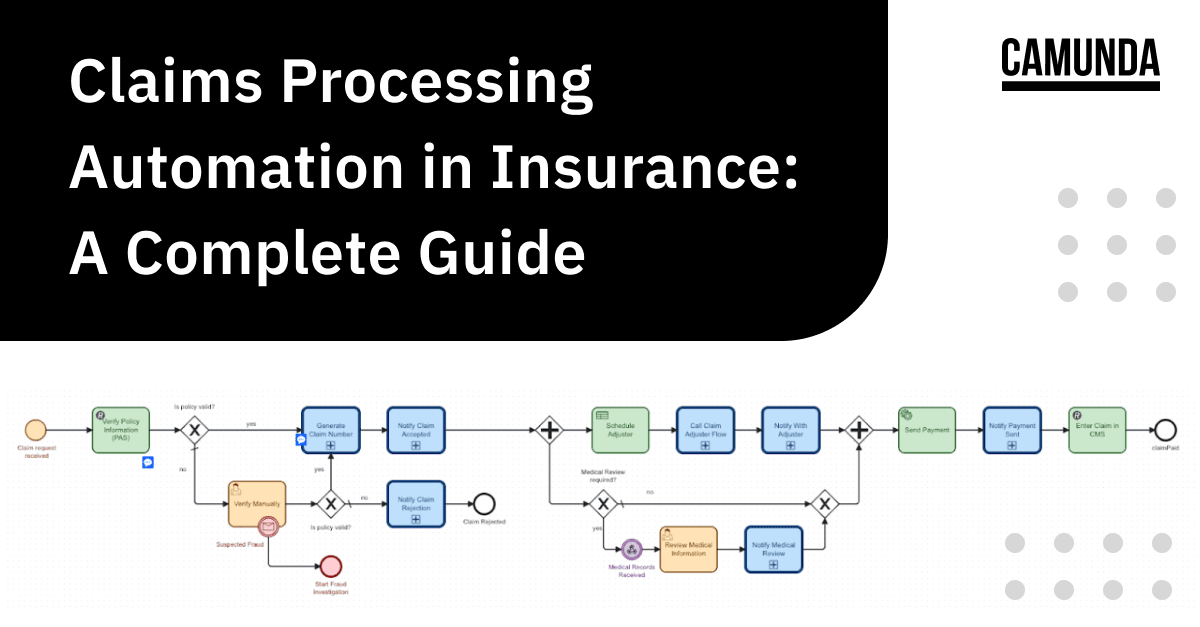
An example of a beginning to a possible automobile claim process might look something like the one displayed below.

This process, represented in Camunda Modeler, shows user tasks in yellow, subprocesses in blue and Connector tasks in green. This diagram illustrates the involvement of the following:
- The customer to initiate the claim by filling out a form
- Policy Administration to verify the policy is effective
- A Connector to generate the claim number
- The adjuster to contact the insured to schedule and complete the estimate
- Accounting to send the payment for the claim.
Along the way, the insured (or claimant) is notified via email of the claim status. Finally, the claims system is updated with the claim details for this customer.
This is an excellent start, but it involves the individual departments working directly in their native systems to complete tasks and doesn’t automate the process effectively.
Well-orchestrated automated insurance claims processing
The following process starts with the previous process and then takes full advantage of Camunda’s strengths, including standard Connectors, gateways, service tasks, webhooks and more.

Let’s dissect this process and how it orchestrates the automobile claim process as implemented with this Camunda process diagram.
To initiate the process, the insured will submit a claim with a form—created with Camunda Forms—that will be filled out with key information about the claim. This is indicated by the circle start event.
The process accesses the Policy Administration System using a REST Connector to confirm that the policy exists in the system. Based on the response, the claim process will be initiated as shown in the top branch, or it will require manual verification in the Claims Department to confirm the policy is valid so the claim can continue.
Using Camunda’s UiPath RPA Connector, a new claim number is generated in the mainframe Claims Management System. In order to properly manage claim cases, Camunda tightly integrates all systems involved in the claims process to provide a holistic view of the customer, the policy and the claim at all times.
In this media age, customers want to opt into status notifications. For this implementation, the process takes advantage of the reuse of subprocesses to provide those notifications as shown by the “notify” blue tasks in the model. The insured is notified throughout the process using both Camunda’s SendGrid Connector for email notification and Twilio SMS Connector for text messaging. Implementing a repeatable subprocess in this manner speeds up modeling and allows the reuse in other process models.

Now that a valid claim number has been generated and initial notifications have been made to the claimant, it is time to schedule the proper adjuster to review the damages and make an estimate on the vehicle repairs.
Using business rules implemented with Decision Model and Notation (DMN) the correct adjuster is selected based on the vehicle and geographical location of the claimant. The adjuster tasks are provided in another subprocess.

In this subprocess, an adjuster estimate form is generated using the Camunda Google Drive Connector with variables from the process to provide the adjuster with a template to use while performing the estimate. Camunda provides an out-of-the-box OpenAI Connector which is used to compose an email to the adjuster the claimant is waiting for an estimate. This email is then sent using our SendGrid Connector.
Simultaneously, a Slack message is made using an out-of-the-box Slack Connector. The adjuster accesses a form that provides a link to the adjuster estimate template created and provides a location to enter the final estimate figure and any specific comments using a human task.
Camunda provides the ability to save Connectors as templates so that the required fields are pre-populated to minimize the need to recreate them each time a configured Connector is utilized within a process.
Going back to the parent diagram—in parallel, if the claimant noted that an injury was involved when the claim was submitted, then the additional medical branch is processed. In claims cases, there are often various assets such as documents, photographs, medical reports and more. Most organizations have implemented an Electronic Content Management (ECM) system to manage these assets.
The process waits for a unique message tied to this claim indicating that the medical documents are available for viewing in the ECM system which is implemented here as a webhook in this process. Once received, the Medical Reviewer can view these documents using the link provided and make comments about the estimate for medical bills in the form provided.

When these branches merge, payment is sent through the Accounting Payment System to the claimant which is implemented as a service task—showing just another method that Camunda offers to integrate systems in your process.
Finally, the Claims Management System is updated with the final results of the claim making sure that all systems are properly orchestrated to manage the claim case.
Continuous process improvement and process insights
Once you have automated your claims process, it is important to be able to get a key understanding of the performance metrics around this process. For example, understanding how the organization is doing against Key Performance Indicators (KPIs) and Service Level Agreements (SLAs). Moreover, with insight into the process, you can also begin to uncover any bottlenecks or areas of improvement to address.
Reports and dashboards can be created that give direct insight into how the process is performing. For example, what the overall processing time is and if any incidents have occurred.

Using dashboards and reports, you can look at data like heat maps that reveal heavy traffic at certain tasks in the process or those that might be taking additional time.


With the data captured, you can begin to look at trends in the process. For example, are certain vehicles involved in more claims than other vehicle types.

You can even begin to look at uneven distribution of work so that it can be streamlined in the future.

Having insight into your process positions you to continuously improve in the future.
The importance of claims processing automation
With a competitive insurance market, organizations must provide a quick and elevated response to claims for customer retention. With a well-orchestrated process, including different messaging options to keep claimants informed, claims can be processed more efficiently and faster. This not only improves customer satisfaction, but also helps to minimize human error and to meet and even exceed existing SLAs.
Try process orchestration and automate insurance claims today
Learn more about how process orchestration can help make your insurance organization run more efficiently and reduce costs, and get started with a free trial today.
Process orchestration for insuranceStart a free trial of Camunda